K2 Deficiency
Even the healthiest diets fall short on delivering all the nutrients the body requires to operate optimally.
It has long been believed that vitamin K deficiency is rare due to dietary intake and contribution from microbial biosynthesis in the gut. Yet published studies show that the majority of both children and adults are vitamin K deficient.
Consider that dietary intake data from the 1950s and early 2000 in the UK show that consumption of vitamin K is now lower than it once was – a likely a consequence of changing diets, as well as food supply. For example, between the 1950s and the 1990s, fats and oils became a larger part of most Western diets than vegetables.
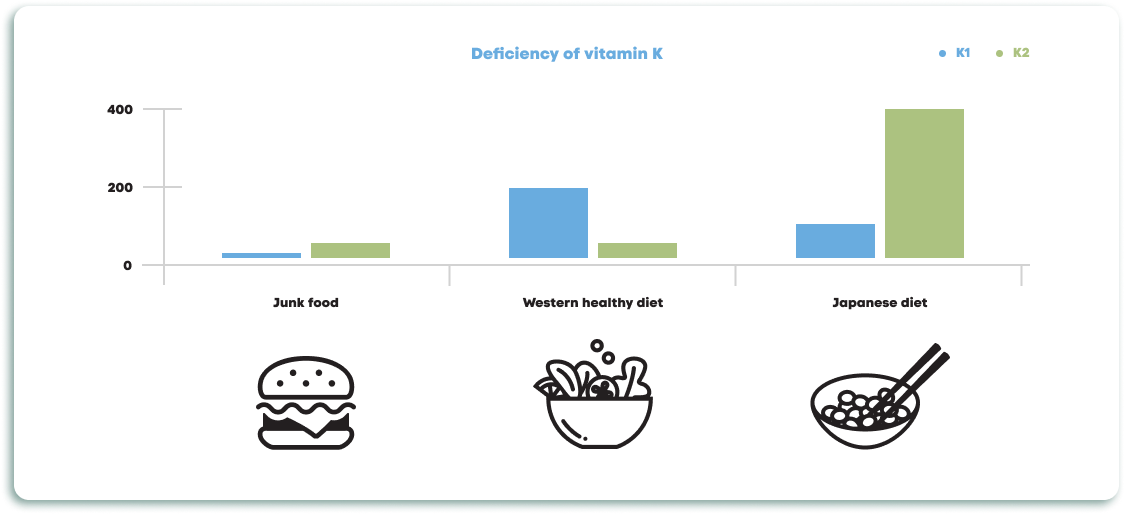
Further, changes in food composition and different preparation practices can also explain deficiencies. Food used to be made in the presence of various bacteria species (synthesizing Vitamin K2). Now, sterile conditions introduced by international standards of food manufacturing stop microorganisms, including beneficial flora, from multiplying and penetrating the human body.
And while it was thought that bacterial synthesis of menaquinones in the colon was a significant contributor to the body’s systemic needs, research now indicates that contribution is much less than previously thought.
Published studies strongly indicate that better Vitamin K2 status contributes to non-calcified, flexible arteries and strong, healthy bones. With a shifting emphasis to fast and processed foods, it is conceivable that vitamin K intakes have been on a significant decline since 1950, which may have serious implications for bone and cardiovascular health.
Vitamin K2 Unrecognized in RDAs
Current daily recommendations for K vitamins are based exclusively on vitamin K1 and the requirement for proper blood clotting, which is presently 1 mcg vitamin K1/kg of body weight (daily). This amount is insufficient for the optimal function of vitamin K-dependent proteins in other tissues like bone and vasculature.
Further complicating the issue is that very few foods contain Vitamin K2 as MK-7. For those that do, we need to eat substantial amounts of those foods daily just to obtain the minimum dosage of 45 mcg to experience any sort of bone or cardiovascular benefit.

